17 Quality Control Testing
Quality control (QC) is typically referred to as the process of monitoring and calibrating equipment, which is just a single aspect of the broader managerial philosophy of quality assurance. Quality assurance encompasses all aspects of patient care, including image production and interpretation, workflow, safety, and radiation protection. While the calibration of X-ray equipment is mainly carried out by medical physicists, quality control technologists can be trained in most of these procedures. It is essential for radiographers to comprehend the necessary types of tests and why certain acceptance parameters are more strict than others, even though they may never perform most of these equipment tests. Every staff radiographer should possess a level of comprehension that allows them to identify problems that may be related to QC and report them to the appropriate supervisor, physicist, or QC technologist.
QC of X-Ray Systems
After the successful installation and acceptance testing of X-ray equipment, it is essential to periodically monitor its performance to ensure that it adheres to the manufacturer’s standards. This monitoring, known as quality control testing, aims to maintain consistent, high-quality diagnostic images, reduce radiation exposure for both patients and staff, and minimize downtime and waste to enhance cost-effectiveness. The quality control program for radiography equipment comprises three parts: visual inspection, environmental inspection, and performance testing. These tests should be conducted when new equipment is accepted or after significant repairs to existing equipment and at least once a year. Any deviations from the manufacturer’s specifications must be corrected or repaired, and records of these corrections or repairs should be kept for inspection by accrediting agencies and state bodies. Similarly, records of QC testing should also be maintained in written form or a computerized database.
Visual Inspection
The key features for performing visual inspection of x-ray systems include checking the main components of the equipment to ensure that there are no hazardous, inoperative, out of alignment, or improperly operating items in the system. This inspection should be performed at least annually with a checklist for documentation. The inspection should include the control console, overhead tube crane, radiographic table, protective lead apparel, and miscellaneous equipment.
Specifically, for the control console, the inspection should verify the proper function of x-ray tube heat sensors and the overload protection indicator, ensure proper functioning of all panel lights, meters, and switches, and ensure a proper view of the exposure room through the window and the presence of an up-to-date technique chart that is displayed near the control panel.
For the overhead tube crane, the inspection should evaluate the condition of the high-voltage cables and other wires, the condition of the cable brackets, clamps, or tie-downs, the stability of the system, proper movement, SID and angulation indicator function, detent operation, lock function, bucky centering light brightness, collimator light brightness, and interlock function.
For the radiographic table, the inspection should inspect the surface condition and cleanliness of the tabletop, power top and angulation switches, bucky tray and cassette locks, stability, table angulation indicator, and the condition of any footboard or shoulder braces. The tabletop material over the bucky area should not absorb more than 1.0 mm of aluminum equivalent.
In addition, lead aprons and gloves should be present in the radiographic room and should have a minimum 0.25 mm of lead-equivalent thickness. Protective lead apparel should be inspected annually for defects such as holes, cracks, and tears. Finally, all inspection results and corrective actions should be documented for accrediting agencies.
Environmental Inspection
The key features of an environmental inspection of x-ray systems include:
- Mechanical integrity: Checking the presence of loose or absent screws, bolts, or other structural elements that may have been improperly installed or have worked loose because of use. Also, checking the functioning of meters, dials, and other indicators.
- Mechanical stability: Checking the stability and stiffness of the x-ray tube support and image receptor, lubricating the moving parts, checking the reproducibility of positioning of the source and image receptor that may be indicated or controlled by physical marks or detents, and checking the accuracy of angulation scale.
- Electrical integrity: Evaluating the condition of the x-ray tube high-tension cables, checking the covering on the outside of the cables, and ensuring that the retaining rings at the termination points are tight and that there are no breaks in the insulation.
- Electrical safety: Checking the physical inspection of the electrical wiring, ensuring all elements are well grounded (to each other and to the ground), and ensuring that all obvious electrical connections are intact.
Environmental inspection should be performed at least annually (it may need to be performed more frequently with older equipment), and it involves general observation of mechanical and electrical integrity and stability. For older equipment or equipment that has a history of problems with electrical safety, a biomedical engineer, medical physicist, or vendor service technician should be consulted for environmental inspections. Many states require that an electrical inspection record be posted on the equipment.
Performance Testing
Performance testing of x-ray systems involves evaluating the performance of the x-ray generator and tube using specialized test instruments. These instruments can range from simple phantoms and tools to sophisticated computerized systems, which are expensive but provide quick and easy data gathering. However, most facilities use several smaller devices to collect the necessary data. The results of these tests must be documented for governmental and accreditation agencies. While a medical physicist is typically required to perform these tests, radiographers should also understand how they are conducted and how to interpret the results.
Radiation Measurement
In conducting performance testing of X-ray systems, reliable measurement of the radiation output is frequently necessary. Gas-filled chambers, including ion chambers, proportional counters, and Geiger-Müller counters, are commonly used for measuring radiation intensity. These detectors work by ionizing gas in the chamber, producing a trail of ions that allows current to flow through the chamber, which is then converted to a voltage pulse that is amplified and counted.
Solid-state or semiconducting detectors are newer models that use a crystal of silicon or germanium with selected impurities added to detect incident radiation. These detectors are relatively small, accurate, and more sensitive than gas-filled chambers.
The radiation reading obtained from these detectors is often the radiation intensity, which is measured in units such as roentgen (R), coulomb per kilogram (C/kg), or gray (Gy). The exposure rate can also be displayed in addition to radiation intensity using rate meters. Detectors can also be calibrated to measure absorbed dosage in rads or grays (Gy).
Testing the Reproducibility of Exposure
An x-ray generator is expected to produce the same amount of radiation each time an exposure is made with the same set of technical factors. This is known as reproducibility. For instance, if a particular set of technical factors produces 300 units of radiation when measured with a dosimeter, then the same set of technical factors used at any later point should also produce 300 units of radiation. The maximum allowable variability in reproducibility is ±5%, according to the regulations set forth in (1020.31(b)), 21 Code of Federal Regulations Subchapter J. Reproducibility can be evaluated by using a dosimeter or a computerized noninvasive system. Reproducibility testing should be conducted after installing new equipment, after significant system repairs, and annually.
We test the reproducibility by using a dosimeter to measure the amount of radiation produced in a series of x-ray exposures made with the same settings. Then, we compare the readings from the dosimeter to see if they are the same each time. The process for measuring reproducibility can look something like this:
- First, a lead apron or sheet of lead vinyl is placed on top of the radiographic tabletop with a dosimeter on top of it. The lead prevents the scatter radiation produced in the tabletop from affecting the readings.
- The central ray of the x-ray beam is then centered on the dosimeter at a source-to-image distance of 40 inches, with the beam collimated so that it is just slightly larger than the dosimeter.
- Next, a series of three to five exposures are made at the same technical factors, 70 kVp and 12.5 mAs, for example. Be sure that the dosimeter is cleared (reset to zero) after each exposure.
- The readings obtained are then recorded on a documentation form, and the reproducibility variance is calculated. To calculate reproducibility variance use the following equation:
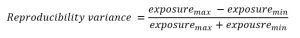
The minimum and maximum exposure readings are obtained from your dosimeter and can be in units of milli-roentgens, μCi/kg air exposure, or mGy of air kerma. The maximum allowable difference, or variance, between the readings is 5%. That means if the first reading is 100, the second reading can be no less than 95 or no more than 105. Variations in x-ray generator performance or x-ray tube operation can arise from malfunctions in the kVp or mA selectors, failure of a rectifier, filament vaporization or tube arcing. When this happens, the reproducibility can be off by more than 5%. This is a problem because it can lead to radiographs of inconsistent quality and potentially require repeat patient exposure to radiation.
